Cardiac rehabilitation has a long standing when it comes to the recovery of individuals suffering from Myocardial Infarction, Cardiac Failure, Coronary Artery Disease etc, continuously demonstrating itself to be among the best therapeutic approaches for boosting the standard of life, lowering problems, and increasing efficiency. When we talk about AI devices as an investment in cardiac rehabilitation we mean by the Artificial intelligence, which offers previously unheard of capabilities in surveillance of patients, customized exercise prescription, potential risks detection, and predictive analytics, is also quickly revolutionizing medicine and rehabilitation.
Table of Contents
ToggleArtificial intelligence is now one of the most revolutionary aspects of cardiac rehabilitation, which has advanced much beyond its conventional exercise-centered concept. AI is already changing ways patients are tracked, evaluated, and assisted during their recuperation process by providing previously unattainable immediate information inspection, customized workout recommendations, early problem diagnosis, and remote monitoring.
AI is bringing accuracy, reliability, and simplicity to cardiac rehabilitation through wearable technology, intelligent algorithms, and digital rehabilitation resources, making it more individualized, accessible, and successful than before. So can your AI driven devices act as an investment in cardiac rehabilitation? Let’s find out.
How different disorders contribute to Cardiac Death?
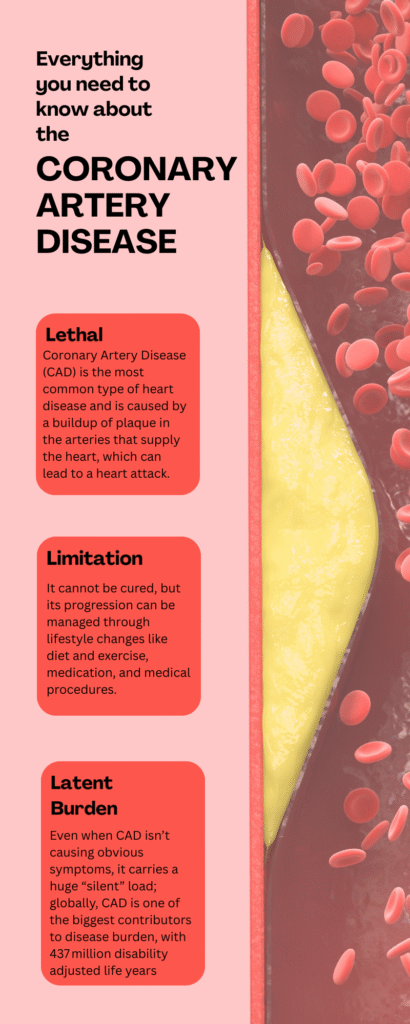
Coronary Artery Disease
Coronary artery disease significantly deteriorates heart health by plugging the circulation to myocardium, which results in both acute & chronic damage. An exceptionally interesting & developing discernment regarding the hemodynamics of the coronary arteries, advocates that the helical circulation which is the blood’s spiraling, whirling motion has two aspects. Significant intensity helical flow can in fact generate areas of extremely high shear stress, increasing plaque vulnerability and the danger of rupture in stenosed vessels, even though certain helical flow may safeguard from minimal shear stress, which is linked to plaque formation.
The conventional wisdom that helical flow is always protective is called into question by this complex knowledge, which also implies that when CAD evolves, the changed flow patterns inherently may exacerbate endothelial damage, hasten atherosclerosis, and eventually collapse plaques.
Myocardial Infarction
Ventricular remodeling is the process by which the heart undergoes significant anatomical and functional changes following a myocardial infarction, which is usually caused by an abrupt, severe blockage of a coronary artery. The immune system’s cells including neutrophils, monocytes, etc, scramble to remove dead cells immediately following MI, but if they are unfettered, they accelerate myocyte death and incapacitate the tissue.
The circumambient myocardium also transposes over time as the injured region is replaced by thickened scar tissue. The extracellular matrix is rearranged and the surviving myocytes grow causing hypertrophy. These alterations result in decreased pumping efficiency and left ventricular dilatation, increased LV volumes, a pattern closely associated with fewer favorable results. Post-myocardial Infarction Cardiac Remodeling: Multidimensional Mechanisms and Clinical Prospects of Stem Cell Therapy

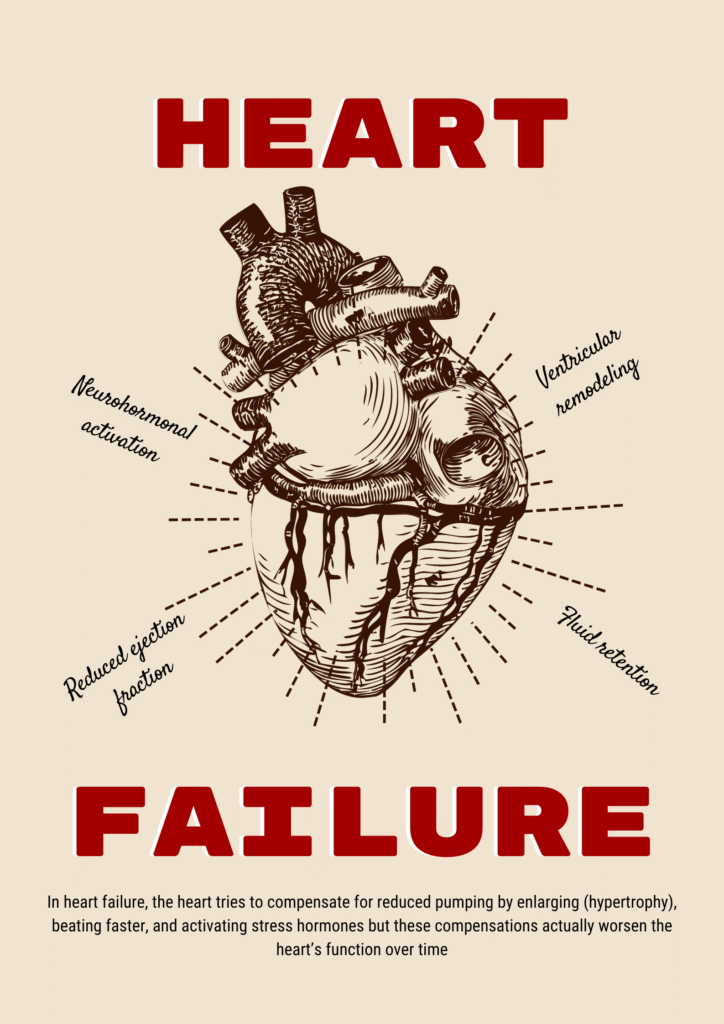
Heart Failure
According to a comprehensive review of heart failure, a HF epitomizes as the end stage of MI or many such disorders. Neurohormonal systems, such as the sympathetic nervous system and the renin-angiotensin-aldosterone system, are periodically stimulated in heart failure as a substitute for decreased cardiac output. However, continuously raised intensity of angiotensin II, aldosterone, and catecholamines promote subsidiary cardiac remodeling. Heart failure is characterized at the cellular level by hypertrophy, fibrosis, oxidative stress, mitochondrial dysfunction, and occasionally cardiomyocyte death.
Numerous issues brought on by heart failure have a significant impact on a person’s everyday life, physical capabilities, and overall wellness. Fluid builds up in the respiratory tract, legs, and belly as the heart weakens and finds it difficult to pump blood efficiently. This results in chronic dyspnea, edema, and a persistent sense of exhaustion that makes it difficult to do even basic tasks like escalating stairs. Additionally, inadequate blood flow lowers the amount of oxygen that reaches the muscles and the brain, which can cause lightheadedness, disorientation, and a decreased capacity for physical activity. Heart failure can increase the likelihood of cardiac arrest over time by causing harmful rhythm abnormalities such as atrial flutter or ventricular arrhythmias.
Chronic reduced circulation also affects the renal system, liver function. and other organs, leading to liver obstruction, decreasing kidney capacity, and electrolyte abnormalities. In the event of excessive fluid intake or abrupt decompensation, patients frequently require hospital stays, which interfere with their ability to perform tasks, communicate with others, and maintain their emotional health. Patients frequently experience anxiety and depression due to physical restrictions, ongoing observation, and erratic symptoms. Heart failure affects every aspect of a person’s life because it produces a cycle of deteriorating organ health, less freedom, and growing hospitalization requirements.
AI Devices as an Investment in Cardiac Rehabilitation
Willingness to use remote patient monitoring among cardiovascular patients in a resource-limited setting: a cross-sectional study, reported that 81.6% of cardiovascular clients stated they would be open to using RPM, or remote patient monitoring, technology. Wearable ECGs, pulse monitoring devices, blood pressure monitors, and trackers for fitness have improved in accuracy and are being utilized more frequently in cardiac rehabilitation and monitoring, according to a 2025 assessment of wearable technologies in cardiology.
The proliferation of contemporary, AI-powered wearable and remote monitoring technologies amply demonstrates their growing value to patient health, particularly in cardiac rehabilitation proving that AI devices can act as an investment in cardiac rehabilitation. They are a crucial addition to conventional therapy because of their capacity to continuously monitor physiological patterns, identify early problems, and offer insights based on data. These tools enable clinicians to make quicker, better informed decisions while empowering patients to remain fully invested in their recuperation.
How do these gadgets monitor data and provide the patient and the physiotherapist with health related updates?
Heart rate, rhythm fluctuations, saturation levels of oxygen, arterial blood pressure patterns, respiratory rate, quality of sleep, and even electrocardiogram signals are all continually recorded by embedded biological sensors in artificial intelligence controlled cardiac monitoring devices. These sensors transform physiological signals into optical or electrical data, which are subsequently processed by onboard algorithms. AI models examine trends, identify abnormalities such as arrhythmias, low oxygen levels, or aberrant exercise reactions, and promptly send out alarms when they find something out of the ordinary. This data is sent to a mobile application or tracking dashboard via wireless or cloud services.
Patients therefore get instant input regarding their heart function, recuperation, degree of physical activity, or possible warning indicators. Patients are able to take control of their exercise, prevent overworking themselves, and maintain greater awareness of their health thanks to this ongoing loop.
By providing precise, frequently collected information that was previously unattainable beyond the clinic, these technologies provide physiotherapists a priceless clinical edge. Physiotherapists can monitor exercise compliance, rhythm adjustments during home cardiac rehabilitation, regular step measures, sleep alterations, or early indicators of cardiac decompensation rather than depending just on sporadic appointments in person or patient recollection.
Numerous technologies produce automated data and statistical charts that assist therapists in remotely modifying treatment programs, identifying danger trends, and adjusting exercise intensity. This results in more individualized, data driven physiotherapy, earlier intervention, and safer rehabilitation. In the end, wearable and AI monitoring devices provide for a more thorough and ongoing assessment of the health of cardiac patients by bridging the gap between the clinic and the patient’s home.
Who can actually wear these devices?
Wearable technology with AI capabilities is becoming more and more recommended for a variety of cardiovascular and respiratory disorders, particularly when continuous surveillance is necessary to avert worsening. In order to monitor exercise response and identify ischemia symptoms beforehand, they are frequently advised for people with coronary artery disease to use both after angioplasty and after bypass.
Instantaneous heartbeat and rhythm tracking, which helps avoid exercise associated with compensatory changes, is very beneficial for patients recuperating following angina, those undertaking cardiac rehabilitation, and those with heart failure or low ration of ejection fraction. These devices are also helpful in tracking different types of arrhythmias or tachyarrhythmias that could be a potential cause of worsening situations.
These devices are frequently used by people with sleeping disorders, hypertension, and chronic obstructive pulmonary disease (COPD) to track blood pressure variations, oxygen saturation, and nocturnal breathing patterns. Moreover, stroke survivors, as well as diabetic patients especially those at risk of developing autonomic dysfunction, can also take advantage of these AI monitoring devices. These devices are also commonly used in telehealth programs, home care rehabilitation, and by patients who need ongoing surveillance where periodic tracking maximizes & ensures the use of safe & sound techniques and therapeutic concordance because they give constant biophysical information.
Exercises that can be Tracked with AI Devices
- Walking or Stair Climbing: Can track slow, brisk or moderate steps & monitor the rhythm of the heart as well as the calories
- Treadmill or Jogging: Useful in monitoring incline ratio and tempo with respiratory rate
- Cycling: Stationary & outdoors can both be tracked using AI devices. Furthermore, these devices can help measure the workload, speed, cadence & distance
- Elliptical Training: Monitors cardiovascular response, heart rate, workout intensity
- Aerobics: Low impact can be tracked along with the fluctuations in heart beat
- Strength Training: Counts steps, reps, intensity, and rest intervals
- Breathing Exercises: Some AI devices can also detect oxygen saturation levels
The Disadvantages of AI Wearables
Notwithstanding their benefits, wearable and AI-powered monitoring systems have a number of significant drawbacks that need to be taken into account. Initially, accuracy of information is subject to variability, particularly when moving, perspiring, or placing sensors incorrectly. This might result in erroneous notifications or overlooked anomalies, which can give patients false reassurance or needless concern.
Numerous devices rely on constant communication and disruptions may result in insufficient statistics that compromise the quality of clinical judgment. Critical biological information is sometimes retained online on unauthorized servers, which increases the possibility of breaches or illegal access, increasing privacy and security issues.
Furthermore, some patients may not be able to purchase premium wearables or services that require monthly subscriptions, particularly in areas with low budget incomes. Some people become overly dependent, which causes them to misinterpret natural swings or check their vital signs obsessively. Additionally, older patients or those who are not comfortable with devices may find it difficult to maintain or properly comprehend equipment readings due to a lack of technological literacy.
Finally, even while AI offers useful insights, algorithms might not always take the whole clinical picture into account, therefore device data should support professional medical evaluation rather than take its place.
What we concluded
All things considered, wearable technology powered by AI is revolutionizing cardiac rehabilitation by providing ongoing, current insight into a patient’s biological state. They are an effective addition to conventional therapy because of their capacity to monitor vital signs, identify early anomalies, and facilitate virtual clinical choices. Although they offer many advantages, including enhanced safety, patient involvement, and customized monitoring, they also have drawbacks in terms of precision, expense, confidentiality, and technological dependence.
In the end, these tools improve the effectiveness of cardiopulmonary rehabilitation, close the disparity among the home sessions and the hospital, and enable clients and physiotherapists to collaborate for a more secured and favorable recovery when utilized properly in conjunction with professional treatment.
This article has been written by a Physical Therapist and provides general guidance on physical health & exercise. While it is grounded in professional expertise, it is not a substitute for individualized medical advice. If you are experiencing pain, specific symptoms, or have an underlying medical condition, please book a 1 on 1, 30 minute consultation with our expert physical therapist for a personalized assessment & tailored recommendations.

Pingback: The Astounding Future of Tele Rehab in ICU -
Pingback: The Hidden Link between Gut Health & Muscle Pain -
Pingback: Is Walking a Part of Exercise Regimen? -