Many of you might be here from the famous Instagram post which states that, “Untreated trauma will turn into dementia. Your body remembers everything your mind tries to suppress.” Well, you are not the only one. The whole purpose of writing this blog, revealing the hidden link between trauma, dementia & physical therapy is to voice out what actually happens when your trauma remains unhealed with time & can physical therapy help such individuals. Let’s find out through some solid evidence.
Table of Contents
ToggleBefore diving into the physiology of dementia, its causes, symptoms & treatment options lets excogitate what we mean by trauma. Childhood trauma which if often termed as Adverse Childhood Experiences (ACE) is defined as the tormenting events before the age of 17 or 18 that may cause severe mental & physical health repercussions.
Types of Traumas Experienced
- Abuse
- Neglect
- Violence either on oneself or on someone in the family
- Substance abuse
- Suicide attempt by a family member or close friend
- Imprisonment of any family member
- Instability after the death of one or both parents
- Vulnerability due to the separation between parents & not adjusting to co-parenting
Numerous additional stressful events may have an effect on one’s health and wellbeing. This can involve coping with homelessness, having insufficient food, or living in precarious housing. Childhood ACEs can have long lasting impacts on a person’s health and well-being, as well as their future prospects in terms of schooling and employment. Physically transmitted illnesses, injuries, and participation in sexual trafficking can all be made more likely by these events.
What really is Dementia?
According to a research, Adverse childhood experiences and risk of late-life dementia: a systematic review and meta-analysis, 47 million individuals were affected with dementia in 2015 & with estimates suggesting that by 2050, this number will triple. Dementia is a neurodegenerative disorder, defined by the decline in cognitive abilities. It isn’t a single disease but a syndrome resulting from progressive neuronal decline in particular brain areas, resulting in a reduction in critical thinking behavior, memory, thought processes, and functional independence.

The Pathophysiology of Dementia
The major pathological change that occurs in dementia is the neuronal degeneration or death. The neurons begin to die or shrink as a result of deposition of toxic proteins, oxidative stress & loss of trophic support such as nutrients, growth signals & survival kits of the neurons. This neuronal degeneration begins years prior to the presentation of actual symptoms & is known as the “preclinical phase of dementia”. Due to this neuronal degeneration, the synaptic connections become weak leading to impaired communication between the various nerve cells. This targeted delay of communication occurs mainly at the level of hippocampus which is responsible for the preservation & regulation of the memory.
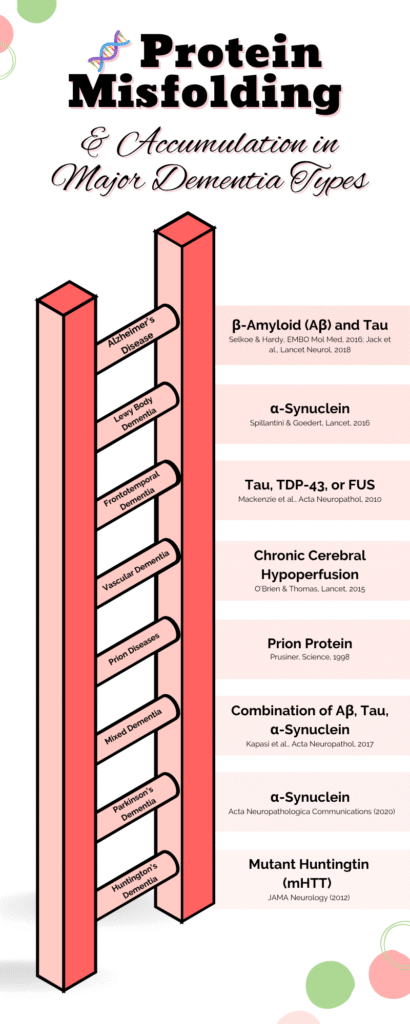
These aberrant proteins clump, misfold, and set off pathways leading to cell death and neuroinflammation. As a result of this neuroinflammation, the microglia which are also known as the brain’s immune cells, become chronically operated. This chronic activation & operation causes the release of cytokines & more inflammation thus resulting in further damage. Eventually, the mitochondria are damaged & less energy is produced. This brings about programmed cell death. The mitochondrial dysregulation is often seen in early Alzheimer’s disease. Moreover, the neurotransmitting capabilities of the receptors is diminished and this results in cholinergic system imbalance which is a cause of memory decline.
Disruptions to the dopamine and serotonin pathways can also occur. In case of non-vascular dementias, cerebral blood flow can be affected by stress, diabetes, obesity, and chronic hypertension. These elements exacerbate neurodegeneration by hastening microvascular ischemia and white matter damage.
Revealing the Hidden Link between Trauma, Dementia & Physical Therapy: Can Unhealed Trauma really cause Dementia?
Neurological connections are formed during childhood, a critical time in human development. Anything that happens during this period may have a lasting impact on health results. The hippocampus and prefrontal cortex, two parts of the brain implicated in cognition and also impacted by childhood stress, have been linked to both structural and functional changes in dementia. These results imply that early life adversities could operate as risk factors for dementia and cognitive impairment in later life. According to a study, Post-traumatic stress disorder as a risk factor for dementia: systematic review and meta-analysis, those who suffer from posttraumatic stress disorder are 1.61 to 1.99 times more likely to develop dementia than those who do not.
Another research, Dementia Risk in Posttraumatic Stress Disorder: the Relevance of Sleep-Related Abnormalities in Brain Structure, Amyloid, and Inflammation, found that the veterans who received a PTSD diagnosis were more than twice as likely as those who did not to acquire dementia in the future. When sociodemographic factors, neuropsychiatric and medical comorbidities, and the number of clinic visits were taken into account, the potential for incidental dementia in the context of PTSD among these veterans stayed noticeably high.
Traumatic life events and risk for dementia: a systematic review and meta-analysis, reported that traumatic life events are associated with increased risk of developing dementia. Oxidative stress, a decrease in hippocampus volume due to trauma, and altered functioning of neurological and psychological pathways such as the hypothalamic-pituitary-adrenal axis may all contribute to an elevated probability of dementia. It may be possible to develop interventions that specifically target these mechanisms and lessen the impact of trauma and PTSD on dementia by acknowledging that PTSD and the detrimental outcomes of TLE are possibly preventable risk factors for dementia.

Interpreting the Evidence
It’s critical to realize that connection does not equate to inevitability. Although a large body of research indicates that people with unresolved trauma or post-traumatic stress disorder (PTSD) are more likely to develop dementia or autoimmune disorders in later life, this does not imply that trauma is the direct cause of these conditions in all individuals. Numerous interrelated factors, including heredity, lifestyle choices, the existence of other disorders, and even the degree of social or medical assistance available, all play a part in the intricate relationship. In plainer terms, trauma does not decide the outcome on its own, but it may be one component that contributes to vulnerability.
Although the biochemical pathways linking trauma and neurodegeneration seem tenable, the relationship is still one of risk rather than certainty, as research published in journals such as SpringerLink and Nature points demonstrated. Practically speaking, this knowledge emphasizes how crucial early intervention and comprehensive health management are. Stress management, trauma treatment, and mental health support are not only psychological issues; they also have significant neurological and physical ramifications. According to the Lancet Commission on Dementia Prevention, dementia incidence can be significantly decreased by addressing modifiable risk factors at every stage of life.
Brain health can be preserved by interventions such as psychotherapy, depression treatment, sleep quality enhancement, physical activity, blood pressure and diabetes management, smoking cessation, and social interaction. Even in those with a history of trauma, these lifestyle and treatment choices can disrupt the biochemical pathways that connect inflammation, chronic stress, and neurodegeneration, providing practical, scientifically supported methods to reduce the risk of dementia.
The Link between Dementia & Physical Therapy
After discussing the correlation between trauma-driven chemical mechanisms and their detrimental effects on brain health, which include how chronic stress, inflammation, and neurochemical disturbances can lead to dementia and cognitive decline, it is equally critical to concentrate on the resolving factor. Physical therapy is a potent, research based strategy that can help in dementia. Let’s find out how.
A research in 2023, The Efficacy and Safety of Physiotherapy in People with Dementia: A Systematic Review, reported that physical therapy approaches such as strength training & aerobic exercises have been linked to improved motor and cognitive results in individuals with dementia. A study in 2020 performed a randomized controlled trial to evaluate whether progressive task oriented circuit training was helpful to improve cognitive function in patients with dementia. The results showed that comparing individuals with dementia to a control group, a 12 week progressive task-focused neurological exercise course enhanced their physical and cognitive abilities. This exemplifies how task oriented neurorehab yields quantifiable results.
Dual-task training, which combines gait & balance activities with cognitive load, has been shown to increase walking speed, balance, and occasionally cognitive scores in individuals with Alzheimer’s disease or dementia. For instance, a 12 week dual task RCT revealed improvements in both cognition and physical function. Dual-Task Training Affect Cognitive and Physical Performances and Brain Oscillation Ratio of Patients With Alzheimer’s Disease: A Randomized Controlled Trial.
Moreover, a recent metaanalysis Effects of motor-cognitive training on cognitive function and gait performance in older adults with dementia ruled out that in dementia, motor and cognitive training and multifaceted exercise demonstrate modest to moderate gains in cognition and more substantial increases in performing everyday tasks.
Can Physical Therapy help Prevent Dementia in individuals with high risk of developing it?
The answer is yes! In older persons at heightened risk, focused lifestyle and exercise interventions can prevent cognitive decline and lower risk of progression, according to large, high quality multidomain trials that include structured physical activity & rehabilitation components. Other evidence comes from FINGER & U.S Pointer which recently reported positive results of large RCT of constructed & proper lifestyle intervention.
According to contemporary neuroscience, movement is the brain’s medication. In comparison to those who stay sedentary, people who participate in organized, regulated physical activity as part of a larger lifestyle initiative exhibit slower cognitive decline and improved brain performance, according to large scale studies like the U.S. POINTER Study (Alzheimer’s Association, 2025) and the FINGER Trial (Ngandu et al., 2015, The Lancet).
This is due to the fact that frequent physical therapy and focused exercise facilitate neuroplasticity, the brain’s innate capacity to create new neural connections, and enhance neurogenesis, the production of fresh neurons in areas like the hippocampus, which is in charge of memory and learning. Read more about Neuroplasticity here at 5 Intriguing facts about Neuroplasticity.
Exercise under physiotherapy guidance improves oxygen and nutrition delivery, preserves cerebral blood flow, and lessens the accumulation of dangerous substances like tau and beta amyloid that are connected to Alzheimer’s disease. These exercises also aid in the regulation of stress hormones and systemic inflammation, two factors that, if unregulated, are known to hasten the aging process of the brain.
Healing the Mind before it Damages the Brain
The increasing amount of evidence unequivocally demonstrates a connection between unresolved trauma and the likelihood of dementia in later life. Whether resulting from stress in adulthood or childhood trauma, emotional anguish can leave behind invisible scars that gently change the chemistry of the brain, impacting memory, emotional control, and overall neural health. Even though not all trauma survivors will go on to acquire dementia, research indicates that chronic anxiety, unhealed emotional scars, and post-traumatic brain changes make people more susceptible. Refusing to suffer in silence is the most crucial step.
The course of your physical and mental health can be altered with early assistance. Each initiative that you make towards mental wellness is also a step in safeguarding your future and mind, even though healing takes time.Physiotherapy provides preventive measures and recovery for people who have experienced trauma or who are already dealing with cognitive decline. Physical therapy promotes neuroplasticity, which enables the brain to create new connections and regain lost functions, through controlled movement, balance training, and neurorehabilitation. Frequent exercise boosts circulation to the parts of the brain that promote memory and attention, lowers stress hormones, and improves sleep.
Through brain and body interaction, physiotherapy can help trauma survivors regain both physical strength and mental stability as part of their comprehensive recovery process. Although brain healing takes time, both the body and the mind are capable of learning to move once again in the direction of strength, balance, and calmness with the correct care, perseverance, and support.
This article has been written by a Physical Therapist and provides general guidance on physical health & exercise. While it is grounded in professional expertise, it is not a substitute for individualized medical advice. If you are experiencing pain, specific symptoms, or have an underlying medical condition, please book a 1 on 1, 30 minute consultation with our expert physical therapist for a personalized assessment & tailored recommendations.

Pingback: The Exquisite Function of Hippocampus & Rehab -
Pingback: Unveiling the Stress Poison & Rehab Recovery -
Pingback: Down Syndrome & Physical Therapy: An Exclusive Guide to Improving Mobility & Independence -